Edited by Mohamad Wehbe
From smallpox in the 1960s to Ebola and Zika outbreaks in 2015 and 2016 respectively, writing the history of human infectious diseases is a long and draining task. With COVID-19 finally loosening its stringent grip over the world after years of fear and tension, humankind has yet to experience another outbreak. SARS-CoV-2 has stolen the spotlight for a while now; nonetheless, it is safe to say that the focus has begun to shift towards another virus on the rise: Monkeypox. With more information surfacing about the most recent outbreak in , the questions and concerns of many can finally be addressed. In light of continuously growing populations and globalization’s exponential exposure of all four corners of the globe to each other, facing newly appearing diseases and fighting viruses has seemingly become a routine. Despite all this, scientific advances and medical knowledge persistently strive to unveil the truths behind these infectious agents and debunk the conspiracies which often arise during times of crisis.
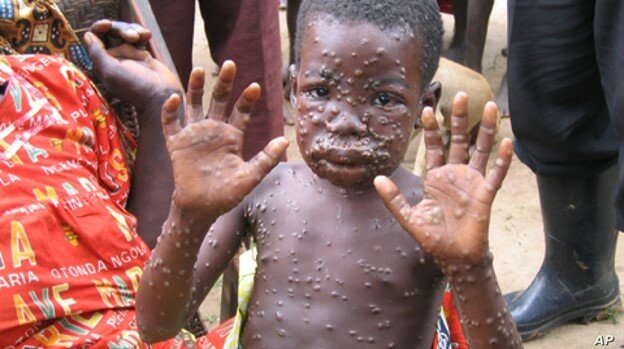
Monkeypox is a rare disease caused by the monkeypox virus which is a double-stranded DNA virus belonging to the Orthopoxvirus genus and Poxviridae family, per the CDC. Related to the famous smallpox virus and probably infecting humans for a very long time, monkeypox was first isolated during 1958 in crab-eating Macaques―a species of monkeys―that were being used for research, hence the name. Yet, monkeypox is actually a misnomer since it most commonly infects small African mammals and rodents, and not just non-human primates like monkeys. It first made its jump to humans in 1970 in the Democratic Republic of Congo (DRC) during a period of solidified efforts aimed at eliminating smallpox, making its way into several central and western African countries as well as America and Europe. Today, monkeypox has spread from endemic countries to Belgium, France, Portugal, Spain, UK, US, etc…even as far as Australia. The eradication of smallpox and “parallel” emergence of monkeypox brings to the table an interesting principle formulated by Dr. James O. Lloyd Smith, professor of ecology and evolutionary biology at the University of California, Los Angeles, called “vacated niches”. “Each pathogen occupies an ecological niche and eradication of one […] leaves a vacant niche that favors the emergence of new [agents] to replace it,” Smith wrote in his . “Extermination can cause a quantitative rise in the incidence of another infection,” he added. Originally, two strains of the virus existed: the “Central African Strain” which could be traced to the DRC, and the “West African Strain” which could be seen in other countries like Cameroon, Gabon, Liberia, etc. This is worth mentioning because the death rates due to infection depend on which strain is circulating. Varying among the two, the former strain recorded a 10% fatality rate while the latter showed figures around 1-3%. A systematic analysis of 48 peer-reviewed articles and 18 literature reviews found that monkeypox cases have increased 10-fold over the past five decades—up from 48 cases in the 1970s to 520 cases in the 1990s.
While monkeypox’s incline has been slow but steady with the Democratic Republic of Congo being the number one contributor, reasons behind the current global outbreak remain unclear. Over the last five years, many monkeypox cases have appeared in at least eleven people returning from Nigeria to various regions of the world, two of which going back to the US in 2021. Further back in time to 2003, forty-seven confirmed cases were also documented in the United States, linked to infected animals imported from Ghana, according to the CDC. So why has the ruckus been raised now when infections like these have always been reported for so long? The answer is that it is only recently that most cases have been documented in individuals that have no connection to countries where the virus could be found nor to animals that could be potential hosts for the virus itself. One possible scenario was proposed by . “Ever since the eradication of smallpox by vaccination in 1980, the shot has been phased out,” she claims. But because the vaccine shows around 85% efficacy against monkeypox as well, the winding down of vaccination campaigns has led to a jump in monkeypox cases, adds Rimoin. While all possible theories are just mere speculations at this stage, studies are underway to further understand the epidemiology and source of infection. In line with this, the topic that raises itself next is the degree of severity of the monkeypox disease and whether the rising concerns are worth the attention or not. , Dr. Jimmy Whitworth―professor of international public health at the London School of Hygiene and Tropical Medicine―assured the public that “this isn’t going to cause a nationwide epidemic like COVID did, but it’s a serious outbreak of a serious disease–and we should take it seriously.” By the same token, a meta analysis of the aforementioned 2003 American monkeypox outbreak revealed very few, if none at all, life-threatening symptoms. The study noticed that people infected with the virus had a rash or skin lesions 97% of the time, fever 85% of the time, chills and lymph node inflammation 71% of the time, and aches around 60% of the time. Normally appearing a week or two after exposure, symptoms often begin with fever, chills, and headaches and progress to rashes and more alarming signs like swollen lymph nodes.
The stages of monkeypox skin lesions. Courtesy: UK Health Security Agency (UKHSA)
Further reinforcing Dr. Whitworth’s pacifying claim toward the seriousness of the infection, experts believe the monkeypox outbreak is unlikely to reach a level similar to that of COVID-19. This is supported by the fact that recent cases from the UK and US which have been taking the media by storm seem to be more related to the West African strain, recording 1% mortality rates and very mild symptoms. In addition, monkeypox being a DNA virus (in contrast to SARS-CoV-2 which is an mRNA virus) means it does not mutate as fast, to the extent that studies have shown current cases very closely related to forms of the virus seen in 2018/19. Compared to Covid, not only is monkeypox a known virus with treatments already established, but also has a slower mode of transmission. Furthermore, containing the virus is easier in the case of the poxvirus because unlike a cough that could be mistaken for a cold in the case of SARS, a distinctive and painful rash a few days after contact makes monkeypox symptoms harder to miss out. However, the World Health Organization’s regional director for Europe, Hans Kluge, has warned that “as we enter the summer season […] with mass gatherings, festivals and parties, transmission could accelerate”. While specialists consider that the general public needs not to be worried at this stage, caution should always be taken especially in young children, pregnant women, and people with weak immune systems. “We always thought Ebola was easy to contain, until that wasn’t the case,” said Prof Adam Kucharski, from the London School of Hygiene and Tropical Medicine.
“The likelihood of a monkeypox pandemic is extremely unlikely”, asserts Aaron Glatt―MD and chair of the Department of Medicine at Mount Sinai South Nassau hospital in New York state. This judgement is largely based on a reliable criterion of virus severity classification; and that is mode of transmission. To begin with, monkeypox virus could be contracted when a person comes into contact with the virus from an animal, human, or contaminated materials, mainly clothing and bedding. On one hand, human-to-human transmission could occur by close contact and large respiratory droplets entering the body through broken skin, respiratory tract, or the mucous membranes such as eyes, nose, or mouth. On another hand, animal-to-human (zoonotic) transmission could take place via close contact, biting, scratching, and infected meat ingestion. “Transmission is really happening from close physical contact, skin-to-skin contact. It’s quite different from COVID in that sense,” said Dr. Maria Van Kerkhove, an infectious disease epidemiologist with the WHO. In contrast to COVID-19 that spreads quickly, simply by talking with another person or sharing a room, contraction of monkeypox requires contact within six feet for a minimum of three hours. That’s quite a long time, a main reason why scientists have overlooked the malignancy of the outbreak and its potential transformation into a more serious pandemic.
While modes of transmission seems a hot topic when it comes to infectious diseases, nothing beats “fake news” on the stage of controversial debates. The race between conspiracy theories and factual evidence is so omnipresent to the extent that the often views its fight against a pandemic as one against an “infodemic” and false information. As has been the case with the Zika virus outbreak, people have created and spread conspiracy theories regarding COVID-19—from its origin and transmission to treatments and cures. The age of social media makes transmission of these conspiracy theories so fast and easy through Twitter, Facebook, and Reddit as to inflict detrimental consequences for the self, others, and society at large. With headlines such as “CDC officials sound alarm for gay and bisexual men as monkeypox spreads in community” and “Gay, bisexual men at increased risk for monkeypox virus” making it to the front page of countless articles and newspapers, the conspiracies around monkeypox have stricken again as anticipated. On Monday, May 23rd, the Centers for Disease Control and Prevention alerted gay and bisexual men that monkeypox appears to be spreading in the community globally, warning them to take precautions. According to an article published by ABC News, the majority of reported UK cases have been detected in gay and bisexual men, leading British authorities to advise these groups to watch out for lesions and any source of possible contamination. However, this is not true. Asexually trasmitted disease experts at the WHO and CDC officials have stressed that monkeypox is not “a gay disease”. Andy Seale, an advisor with the HIV, hepatitis, and sexually transmitted infections program at the WHO, highlighted just that. “While we’re seeing some cases amongst men who have sex with men (MSM), this is not a gay disease as some people on social media have attempted to label it. That’s just not the case. Anybody can contract monkeypox through close contact,” emphasizes Seale. Since respiratory droplets generally cannot travel more than a few feet, prolonged face-to-face contact often provided by intercourse paves the way for viral infection. In Seal’s view, MSM communities tend to be more likely to approach health services when encountering sexual health concerns, which may explain why monkeypox cases have been identified in these communities. The stigmatization of homosexuals is further heightened when an article published in The Telegraph declares sources telling the journal that a gay party in Spain is also being advertised as the root cause of the global monkeypox cases. With the latter still a blunt accusation, journalist Joe Pinkstone attributes most cases in Spain to a superspreader event at an adult sauna in Madrid. , claimed that health officials had traced many of Spain’s 30 monkeypox cases to a single sauna in the capital. What’s more delusional are the conspiracies around bioterrorism and theories that the United States let the poxvirus loose to swirl in China, as mentioned in . , who has 6.41 million Weibo followers, deliberately uploaded the following quote on the platform: “a plan by the US to leak bioengineered monkeypox virus.” The post was liked by more than 7,500 users and received more than 660 agreement comments. Nonsense of this sort has been rife in China and the US since the Covid pandemic, with the two countries engaging in unsubstantiated claims over the origins of the SARS-CoV-2 and monkeypox viruses.
“We want to help people make the best informed decisions to protect their health and that of their community from monkeypox,” says Dr. John Brooks, a CDC official. This infectious disease is not COVID—in a good way. It is not respiratory spread that is the predominant worry, but contact instead. Although the recent transmission of monkeypox cases is alarming, the virus is far less contagious than COVID-19, according to Jo Walker, an epidemiologist at Yale School of Public Health. It is believed that the spread of monkeypox between humans is not efficient enough to sustain itself without constant introduction from zootic populations. This is a main pillar of confidence for the WHO that firmly believes that cases of this disease will not abruptly skyrocket. It is not a sexually transmitted disease, nor is it a bioweapon engineered by the world powers by any means. It is a rather containable situation. Because monkeypox and smallpox are closely related, “we have the benefit of all those years of research, diagnostics, treatments, and vaccines that will be brought to bear upon the situation now,” said Dr. Rosamund Lewis of the WHO. Fortunately, some nations, including the United States, have even stored smallpox vaccines in reserves in case the endemic ever reemerges. Now, FDA approved vaccines, ACAM2000 and Jynneos, can hopefully be used to contain this monkeypox outbreak.
The COVID-19 pandemic has changed the way the public reacts and talks about infectious diseases. The case of monkeypox is not much different. Although ample research must still be undertaken to better understand these ever-changing and evolving pathogens, the best thing to do at the moment is lean on the information scientists and researchers have already brought to life. With billions of people suffering from malicious diseases worldwide, scientists are on alert to prove once again that they are our beacon of hope…even during the darkest times.